St. Lawrence Dentistry is fortunate to have many senior patients, and we strive to do our small part in helping them maintain and elevate their health.
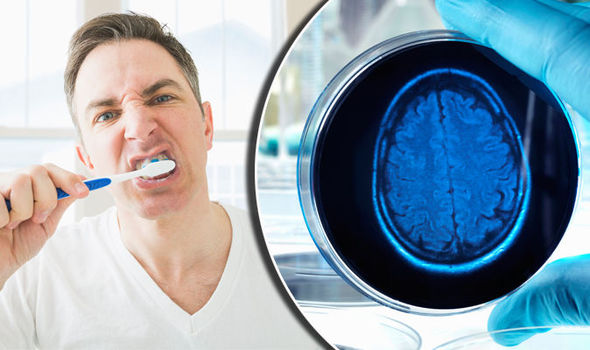
With advanced age comes some challenges, and Alzheimer’s disease is one of them. Research keeps evolving, and a landmark study suggests a link between mouth bacteria and Alzheimer’s disease.

After years of frustration, there are new leads on the research of Alzheimer’s disease. Interesting correlations have emerged, suggesting that the cause of the ailment is bacteria highly involved in gum disease. Understanding this association could prove to be of pivotal importance in developing treatments for this enigmatic condition.
To learn more about gum disease, please visit us here:
In the past, dementia was not as common since people did not live as long. Now it is the fifth most prominent cause of mortality. Alzheimer’s makes up more than two-thirds of dementia cases. This unfortunate sickness is characterized by declining memory and thinking ability over a decade or so. Many of us can relate as we have had family members afflicted which this shattering condition. It is no short of devastating to both those who have it and their loved ones.

Alzheimer’s disease is associated with the gradual gathering of 2 types of proteins—called amyloid and tau — in the brain. These form overarching sticky plaques in the brain’s vital centers. However, some people in their late eighties and beyond have brain plaques without having cognitive issues- this has recently led researchers to debate whether these proteins have a distinctive role in Alzheimer’s disease.

In 2016 investigators reasoned that the role of amyloid seemed to be a sticky protective layer against bacteria. They found that the protein can function as an anti-microbial compound that neutralizes bacteria. At that time, researchers thought that the amyloid went on to give rise to the brain damage of Alzheimer’s, not bacteria. However, the general opinion on this now is transforming. Bacteria are in the brains of individuals with Alzheimer’s. However, it has not been clear whether the bacteria caused the disease or they were able to gain access to the brain impaired by Alzheimer’s.

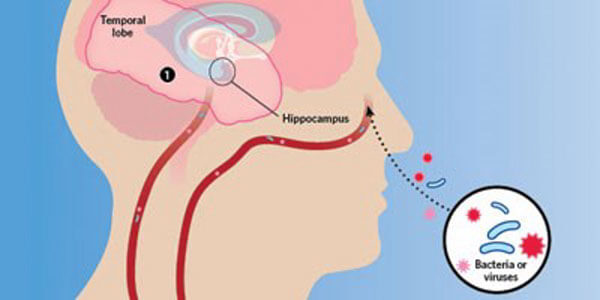
Porphyromonas gingivalis is the primary bacteria found in gum disease and is a known risk factor for Alzheimer’s. So far, researchers have found that P.gingivalis spreads into and inflames brain regions affected by Alzheimer’s disease. In Alzheimer’s patients, investigators found two harmful enzymes P.Gingivalis uses to feed on human tissue in over 95% of brain samples taken from the hippocampus part of the brain— the region critical to memory. Furthermore, Alzheimer’s patients have genetic material from P.gingivalis is found in their brains brain’s cerebral cortex, which is essential for conceptual thinking. Researchers postulate that P.gingivalis enters the brain due to Alzheimer’s and could be a part of the disease genesis.

Experiments involving mice have also shed light on this subject. Research teams infected mice with gum disease, which lead to brain infection, amyloid production, tangles of tau protein, and neuron damage- this seems to demonstrate causation.

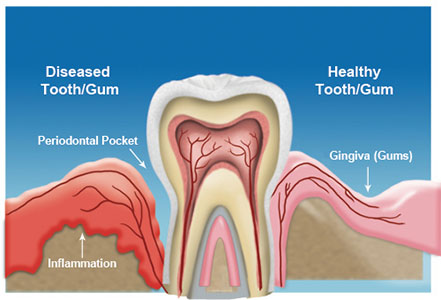
It is unknown exactly how P.gingivalis accesses the brain. There are feasible courses it could take. When plaque forms at the edge of your teeth, it causes periodontal pockets in which P.gingivalis can flourish and secrete toxins. This inflammation can culminate in bone and tooth loss. Some investigations have demonstrated that people with fewer teeth have an increased probability of dementia. The inflammation and toxins secreted by P.gingivalis degenerate the lining of your mouth, which makes it easier for bacteria to infiltrate the bloodstream and invade other organs.
In health, the blood-brain barrier helps shield against microbes. However, P.gingivalis can diffuse into white blood cells and may enter the brain in that manner. They also may attack cranial nerves near the mouth, then metastasize from cell to cell toward the brain over the years.
There are two main ideas on how P.Gingivalis may cause dementia. It may prompt the release of amyloid. The amyloid may incase the bacteria in an attempt to contain the infection. The encasement may also, unfortunately, suffocate and kill neurons. Another possibility is that P.gingivalis may directly damage the brain. The medical community recognizes that Alzheimer’s involves inflammation in the brain, which annihilates neurons. P.gingivalis is known to cause inflammation of the gum tissue, and it may do the same in the brain.
Other researchers have expressed reservations about a possible link of Alzheimer’s to gum disease, saying that a person’s genes are what onsets Alzheimer’s. However, this bacterial postulation does not conflict with this as the combination of genetic and bacterial status may mix to determine a person’s susceptibility to the disease. A natural question asked is if the bacterial hypothesis is correct, would our ancestors have had more incidence of dementia? – due to less oral care in antiquity. However, in previous generations, life expectancy was far less. Hence people did not live to the advanced age at which Alzheimer’s is more common.

It’s too early to tell if the correlation between mouth bacteria and Alzheimers indicates causation. However, it is prudent to do everything possible to prevent gum disease. Cleaning your teeth twice a day, flossing, or using interdental sticks to remove plaque can be of great help in preventing gum disease. It is important not to brush too hard as this may usher bacteria to enter your bloodstream. If plaque accumulates, it can turn into hardened calculus, which encourages the growth of more plaque. It is difficult to remove calculus by regular brushing. Fortunately, a dental hygienist can easily remove this unwanted calculus.

To learn more about dental cleanings at St. Lawrence Dentistry, please visit us here.
We hope you have found this article informative. Please give us a call if you live in the Mississauga area to further investigate how your oral health may affect your total health.
Reference: New Scientist Feb/2019
- Sleep Dentistry: Enhancing Comfort and Care During Dental Procedures - July 11, 2024
- The Revolutionary Injection Molding Technique for Composite Veneers - June 27, 2024
- Why Are Third Molars Called “Wisdom Teeth”? - June 19, 2024