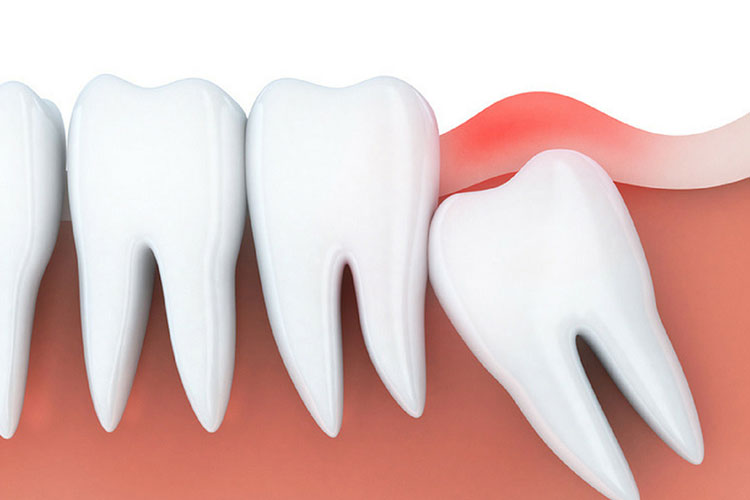
26% of the population has suffered from orofacial pain at some point.
It can be either odontogenic (coming from teeth) or non-odontogenic. Cracked mandibular (lower) molars are the most common source of unexplained orofacial pain.
The perception of orofacial pain is intricately related to understanding the trigeminal nerve. It is the part of the nervous system responsible for sending pain, touch, and temperature sensations from your face to your brain. The 3 main sensory branches of the trigeminal nerve are: (V1) ophthalmic branch, which innervates the forehead and eye, (V2) maxillary branch, which innervates cheek and upper lip, and (V3) mandibular branch, which innervates the lower face and jaw. Other nerves can also cause head and neck discomfort. For example, the innervation of the posterior part of the head is by the 2nd and 3rd cranial nerves. In addition, the glossopharyngeal nerve innervates the rear part of the tongue.
We can classify the acute types of oro-facial pain in the following categories:
- Odontogenic or non-odontogenic
- Atypical odontalgia
- Sinusitis
- Migraine
- Cluster headache
Odontalgia means tooth pain. There is a relationship between odontogenic pain and dentoalveolar pathology. Therefore, we can eliminate it by local anesthetic injection. Examples are teeth abscesses or a dry socket. Non-odontogenic pain is non dentoalveolar pain. Examples include aphthous ulcers, TMJ disorders, burning mouth syndrome, salivary gland infections, necrotizing ulcerative gingivitis, and sinusitis.
Neuralgias as also sources of non-odontogenic pain and include:
- Tic Douloreaux: triggered by touch, chewing, or brushing (related to cranial nerve 5)
- Glossopharyngeal pain: (related to cranial nerve IX) triggered by swallowing, coughing, sneezing, or ear pressure

In terms of pain management, the pharmacological approach aims to optimize analgesia. The first step is for Dr. Hawryluk to determine the etiology (cause of the pain). He will determine if the pain caused is an infection, trauma, or something else. We need to consider the patient’s age, cardiovascular function, renal function, and whether or not they are immunocompromised.
If there is an infectious cause, we have to consider the use of:
- Topical antibiotics, such as chlorhexidine (Peridex)
- Topical antiseptics, such as sodium perborate (amosan) – which is very effective but strangely rarely used by dentists
- Combined topical antiseptics/analgesics such as benzydamine (Tantum)

If topical antibiotics are not sufficient, we have to use systemic antibiotics. The length of therapy usually lasts 7-10 days when appropriate. The only thing you achieve with short-duration antibiotic use is an adverse outcome- antibiotic resistance.
Examples are:
- Amoxicillin 250-500mg p.o every 8 hours
- Amoxicillin/clavulanate (500mg amox, 125mg clav, p.o, every 8 hours)
- clarithromycin (250-500mg) p.o every 12 hours — if patients allergic to penicillins
To learn more about antibiotics in dentistry, please visit us here:
https://www.stlawrencedentistry.com/blog/dental-health/antibiotic-use-in-dentistry/

In addition to antibiotics, some patients will need medications to help with pain during dental infections. Children are a special group when considering pain control. Some common children’s pain medications prescribed (after a though in-person exam) are:
For children in mild to moderate pain;
- 12 years or younger: acetaminophen 12-15mg/kg q4h (max of 65 mg/kg/day)
For moderate to severe pain;
- 12 years or younger 10mg/mg q4-6h ibuprofen
- over 12 years 200-400 mg q4h ibuprophen
If possible, St. Lawrence Dentistry will manage dental discomfort without using opioids. “Codeine” is not approved for children 12 years and under in Canada. The FDA does not recommend codeine for patients under 18 years old
We hope you have found this article informative. If you’re looking for a new dentist in Mississauga, please call us!
Reference:
UTooth.ca (2022)
- Sleep Dentistry: Enhancing Comfort and Care During Dental Procedures - July 11, 2024
- The Revolutionary Injection Molding Technique for Composite Veneers - June 27, 2024
- Why Are Third Molars Called “Wisdom Teeth”? - June 19, 2024