In dentistry, several sources of dental discomfort are unrelated to a tooth being infected or inflamed.
This article spotlights two of these: atypical odontalgia and sinusitis. We have defined the words marked in (*) at the end of the article.
Atypical odontalgia is tooth pain without an identifiable cause. It is also called as “persistent idiopathic facial pain”, “non-odontogenic tooth pain”, and “neuropathic oral-facial pain”. To diagnose this enigmatic condition, we have to establish whether the pain occurs in a tooth that is diseased or a healthy tooth.
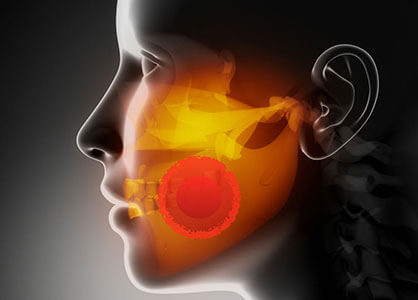
The signs and symptoms of atypical odontalgia pain are:
- Typically unilateral and persistent.
- Poorly located, the location may change with time.
- Frequently in the nasolabial fold or side of the chin.
- Does not follow a dermatomal distribution(*).
- May extend to the upper or lower jaw.
- May extend to a broader face or neck.
- Not accompanied by autonomic nervous system(*) signs and symptoms (such as redness, lacrimation, tearing of the eyes).
There is no accompanying dental pathology or abnormal imaging/lab results with this condition. It is often heterotopic (referred pain) and non-responsive to local anesthetics. Therefore, we must evaluate the underlying psychosomatic(*) disorders such as stress and anxiety when dealing with this pain type. It can be episodic or continuous.
Some cardinal signs of non-odontogenic tooth pain are:
- Spontaneous multiple toothaches.
- Inadequate local dental causes the pain.
- Burning, non-pulsatile toothaches.
- Constant, unremitting toothaches.
- Persistent, recurrent toothaches.
- Local anesthetic blocking the offending tooth does not help.
- Failure of toothache to respond to reasonable dental treatment.
Temporomandibular disorders and neuropathic pain are the most common etiologies of non-odontogenic orofacial pain. In addition, the cause of some non-odontogenic is medications such as risperidone, quetiapine, and aripiprazole.

Treatments include for atypical odontalgia include:
- cognitive behavioral therapy.
- Stress coping techniques.
- Acupuncture, physiotherapy, hypnosis.
- Sphenopalatine ganglion blocks(*).
- cannabinoids.
- First-line medications include tricyclic antidepressants such as amitriptyline.
- Second-line treatments include Prozac, Effexor, Tegretol.

Sinusitis is an inflammation of the mucosa lining the sinuses. The sinuses are four paired spaces in the skull with narrow channels connecting them. This drainage assists keep the nose hygienic and free of microbes. Generally filled with air, the sinuses can get occluded and filled with fluid. When that happens, microbes can grow and cause an infection (bacterial sinusitis).
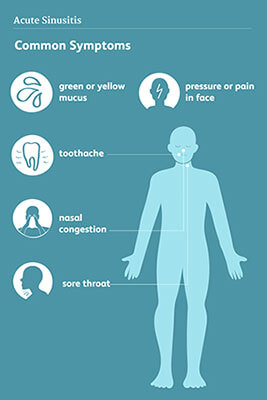
Sinusitis pain is often:
- Constant, dull, boring.
- In the zygomatic region.
- Can be unilateral or bilateral.
- Pain increases with position.
- Radiates to upper teeth and forehead.
- Purulence of the nasal cavity.
- Common around upper respiratory infections.
The etiology of sinusitis can be viral, bacterial, or allergies. Odontogenic infections account for about 10-40% of sinusitis. Nasal decongestants such as pseudoephedrine can help. Sometimes antihistamines(*) such as diphenhydramine are beneficial. Nasal steroids such as fluticasone can help. We do not use antibiotics to treat sinusitis if symptoms have only been present for less than ten days. The exception is high-risk patients who would revive antibiotics immediately.
St. Lawrence Dentistry hopes you have enjoyed this article. Thank you for reading it!
Glossary:
- Dermatomal pattern – patterns of sensory nerves that cover various parts of the body.
- Autonomic nervous system -a portion of the nervous system that unconsciously modulates bodily functions.
- Psychosomatic disorder – a disease that involves both mind and body.
- Sphenopalatine ganglion block – a technique in which a local anesthetic is administered to the sphenopalatine ganglion (SPG)—a group of nerve cells situated behind the nose—to alleviate headache pain.
- Antihistamines – a class of drugs typically used to treat symptoms of allergies.
Reference:
UTooth.ca (2022)
- Sleep Dentistry: Enhancing Comfort and Care During Dental Procedures - July 11, 2024
- The Revolutionary Injection Molding Technique for Composite Veneers - June 27, 2024
- Why Are Third Molars Called “Wisdom Teeth”? - June 19, 2024