When people hear of the phrase dead tooth, they often think of Halloween or something ominous. However, rest assured, it is fortunately easily treated if attended to early.
What is a dead tooth?
A dead or non-vital tooth is a tooth that has no access to blood flow. A healthy tooth contains pulp tissue in the center of the tooth; composed of nerves, blood vessels, lymph tissue, and connective tissue. Lymph tissue plays a role in transporting white blood cells, and the vascular tissue is responsible for transporting other components of our immune system, which keeps the inside of a tooth sterile and healthy. A “dead pulp” means no pulp tissue is present in the tooth, and hence there are no immune cells present to keep the tooth free of bacteria. Whenever a warm moist environment is inside a tooth devoid of immune cells, bacteria will often find a way to accumulate, resulting in a tooth’s bacterial infection.

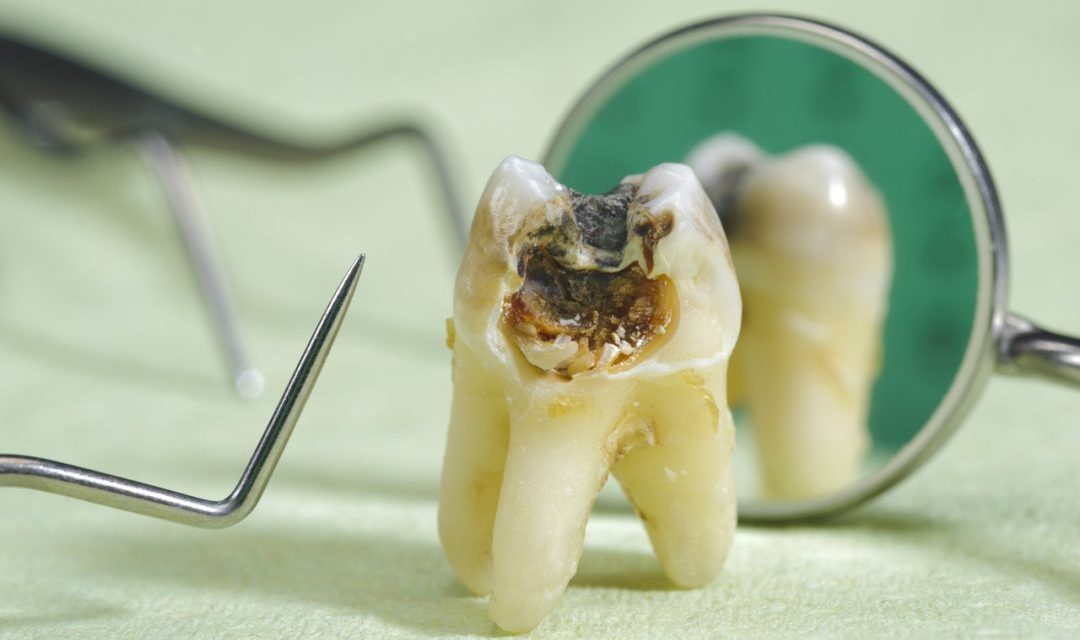
Untreated tooth decay is the most prevalent cause of a dead tooth. When a dental cavity gets very large, it may reach the tooth’s inner pulp layer, resulting in pain and inflammation. Eventually, the tooth’s pulp may become necrotic because the swelling is too much for it to handle. The dental pulp responds to decay by trying to protect itself by constricting its vessels. Consequently, the pressure inside the tooth increases, leading to less (and eventually no) blood flow.

To learn more about dental decay and its treatment, please visit us here:
Caries/Cavities Dental Treatment
Any form of a “physical knock” on the tooth can result in a dead tooth. Tooth trauma can result from sports injuries, falling on your front teeth, and severe grinding. When knocked, the blood supply at the tip of the root can be severed, causing the pulp to die. To protect against this, St. Lawrence Dentistry recommends Sports Mouth Guards for contact sports. A custom-fitted sports mouthguard can protect against dental trauma better than a standard boil and bite one found in sports stores. Dr. Hawryluk Sr. was the dentist for the Toronto Maple Leafs Hockey Club for many years, so he has ample experience making sports guards.

Not every traumatic incident results in a tooth losing its vitality. After tooth trauma, Dr. Hawryluk will assess the area and see if further treatment is necessary. Sometimes the blood supply to the tooth is only temporarily disabled; hence, diagnosing a dead tooth may take several weeks to make definitively. The tooth can often be mildly symptomatic for a few weeks and then tighten up over time. Waiting to see what happens over time can avert the need for root canal treatment. Dr. Hawryluk has ample experience with teeth in these circumstances and will ensure an accurate diagnosis.
How to Identify Dead Tooth?
It’s not easy to identify a dead tooth by just looking at it. One main symptom of a dead tooth St. Lawrence Dentistry looks for is tooth darkening. A tooth with a yellow, grey, or black shade is a sign of a dead tooth. The discoloration is sometimes due to bruising from dying blood cells. Dr. Hawryluk can return your tooth to the proper shading by dental bleaching or a porcelain crown application.
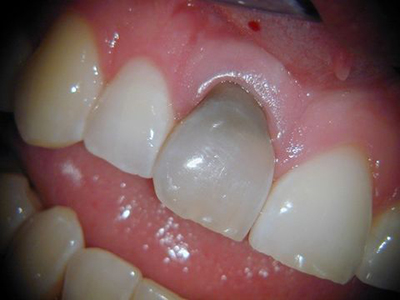
Dr. Hawryluk said that the most common tooth to become non-vital is the primary upper central incisor in children. Children around 3-5 years often fall, and these teeth get knocked a lot. Parents often come in distressed to see their child’s tooth becoming dark. Fortunately, in many cases, no treatment is needed, and the tooth will naturally exfoliate around 7-8 years of age. Treatment on these primary teeth may be required if the tooth remains tender, a bubble forms around the tooth’s root area, or if it is mobile. An x-ray can help make a diagnosis, and the treatment options may include removing the primary tooth and or cleaning out the root of the tooth (primary pulpotomy).
Dead Tooth Symptoms
Pain is a common symptom of a dead tooth. It can vary, from mild, non-existent, to more severe. When the tooth pulp dies, bacteria build up in the tooth, and this eventually can spread outside of the tooth at the end of the root creating a dental abscess. The pressure a tooth abscess puts on the ‘periodontal ligament’ is responsible for the pain. If an infection is present, you may notice a sour taste, swelling, altered smell of the area, or a pimple on the gum. Dr. Hawryluk will be able to tell you if these signs are a manifestation of a dead tooth. An x-ray will often show a radiolucency at the end of the tooth. The “lucency” represents where the abscess has eaten away the bone and replaced it with bacteria-laden tissue (dental abscess). The dead tooth may eventually loosen up and be tender to percussion and chewing.
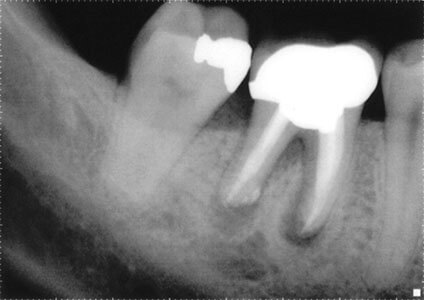
Dead Tooth Treatment
Root Canal Therapy is the primary treatment needed to retain a dead tooth that has become infected. A root canal thoroughly cleans out and sterilizes the middle part of the tooth, which once contained the dental pulp. After cleaning the bacteria, the root is filled “obturated” with Gutta Percha, a rubber, which completely seals the canal space. At the end of the root canal treatment, there should be no bacteria left in the tooth. Some lingering discomfort may be present for a few days due to inflammation/infection of the surrounding tooth tissues. However, once the root is ‘corked-off,’ the surrounding bone’s immune cells can usually start to dissipate and eventually rid the bone of bacteria. At St. Lawrence Dentistry, we use the latest technology, and Dr. Hawryluk Jr. has done thousands of successful root canals. One indispensable part of our treatment armamentarium is the Global Dental Microscope. With it, Dr. Hawryluk can see with unprecedented clarity, ensuring no canal space is left unfilled. If the abscess does not heal from the root canal treatment alone, sometimes simple endodontic surgery (apicoectomy) is needed to clean any remaining abscess tissue in the bone.
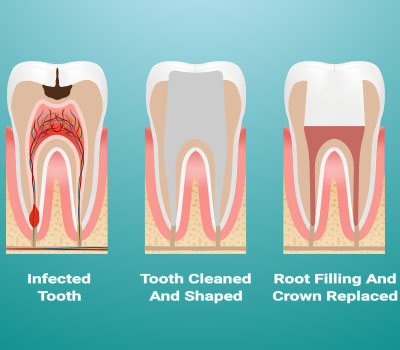
To learn more about root canal procedures at St. Lawrence Dentistry, please visit us here:
Root Canal Procedures Can Save Teeth
To learn more about apicoectomy (root-end) procedures, please visit us here:
Apicoectomy: “Root End Procedure that Can Save Teeth
I f you feel you may have a tooth with is dead and would like to confirm your assumptions, please call the reception desk at St. Lawrence Dentistry. They will book a consultation with Dr. Hawryluk Jr., and he will see what the status of your tooth is. We will do several tests, which may include percussion, heat, and cold sensitivity tests. We will see if any abscess tissue exists around your tooth and discuss treatments to eradicate it.
If you feel you may have a tooth that is dead and live in the Mississauga area, please call the reception desk at St. Lawrence Dentistry. They will book a consultation with Dr. Hawryluk Jr., and he will see what the status of your tooth is. We will do several tests, which may include percussion, heat, and cold sensitivity tests. We will see if any abscess tissue exists around your tooth and discuss treatments to eradicate it.

Sometimes dead teeth need to be removed. To determine if tooth removal is the best option, Dr. Hawryluk Jr. will consider the probability of success with repair options, whether there is a need for additional procedures like crowns, the length of the roots, and the position of the tooth in the mouth. Removal is a practical option for some people with budget restrictions, as this is the least expensive procedure. The extracted tooth can be replaced later by a dental implant, partial denture, and in some cases, a fixed bridge.

To learn more about tooth extractions, please visit us here:
To learn more about the tooth replacement discussed above options, please visit us here:
Choosing between Dental Implants or Bridge Treatment
A Dead teeth can lead to a dental abscess, and the rate at which they can ‘flare up’ can catch people by surprise. Since having a beautiful set of teeth is an asset to our overall health, taking care of any non-vital teeth is an investment in your well-being. If you live in the Mississauga/Oakville area and think you may have a dead tooth, please call our office.
- Sleep Dentistry: Enhancing Comfort and Care During Dental Procedures - July 11, 2024
- The Revolutionary Injection Molding Technique for Composite Veneers - June 27, 2024
- Why Are Third Molars Called “Wisdom Teeth”? - June 19, 2024